Molecular Diagnostics: Revolutionizing Health Testing
Molecular diagnostics has changed how we detect and understand disease. It looks at illness at the DNA, RNA, and protein level, which gives labs and clinicians a much clearer view of what is happening in the body. By combining molecular biology with diagnostic testing, it helps improve patient care.
Techniques like PCR and next-generation sequencing sit at the center of this work. They support earlier detection, more precise diagnosis, and treatment plans that fit the patient better. That is a big reason molecular diagnostics now plays such a large role in clinical diagnostics and precision medicine.
Biomarker analysis and genetic testing are also key parts of the field. They help identify disease states and inherited risk. That information can shape treatment choices and improve outcomes.
Molecular testing keeps moving fast. It gives labs ways to test that are accurate, fast, and often less invasive. These tools are changing both lab diagnostics and day-to-day patient management.
Demand for better diagnostic tools keeps rising. As the technology improves, molecular diagnostics will keep expanding its role in healthcare. The goal is simple: better outcomes and more efficient care.
What Are Molecular Diagnostics?
Molecular diagnostics studies biological markers in a patient’s genetic material and other molecules. It uses advanced methods to detect specific sequences, mutations, or patterns linked to disease. Molecular biology is the base that makes these tests possible.
These tests focus on changes at the molecular level, including DNA, RNA, and proteins. That helps labs spot genetic variation tied to disease and gives clinicians more exact information for diagnosis and treatment. In practice, that means better decisions and better patient management.
Some of the main features of molecular diagnostics include:
- analysis of nucleic acids and proteins
- detection of genetic mutations and molecular changes
- personalized health insights based on the patient’s biology
One reason molecular diagnostics matters so much is speed and accuracy. It can help detect disease before symptoms appear. That gives clinicians a better chance to act early and choose treatments that fit the patient’s biology.

Key Molecular Diagnostic Techniques
Modern molecular diagnostics relies on several advanced methods. These techniques help identify genetic and molecular changes that drive disease. They also help guide treatment decisions.
PCR, NGS, and microarray analysis have changed lab diagnostics in a big way. They offer strong sensitivity and precision, and their impact on patient care keeps growing as the tools get better.
Polymerase Chain Reaction (PCR)
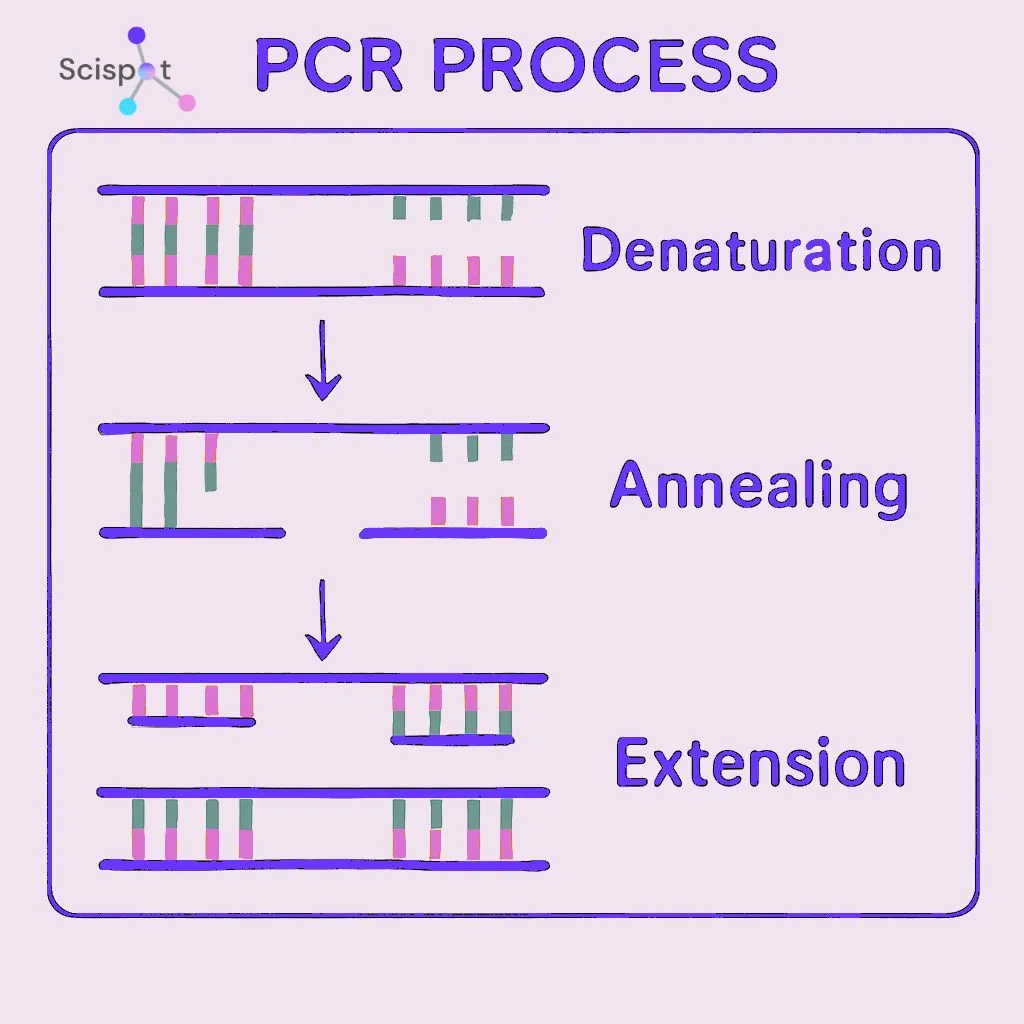
PCR is one of the best-known tools in molecular diagnostics. It amplifies tiny amounts of DNA so they can be studied in detail. That makes it useful for detecting genetic mutations and infectious agents.
PCR works through repeated cycles of heating and cooling. Each cycle copies the target DNA, and the process quickly builds millions of copies. Labs use it widely because it is reliable, efficient, and well suited for both genetic testing and pathogen detection.
Some clear advantages of PCR are:
- high sensitivity
- strong target specificity
- fast results
Clinical diagnostics depends heavily on PCR because it is both accurate and practical. It has been widely used for viral detection, including COVID-19, and it remains one of the core tools in molecular testing.
Next-Generation Sequencing (NGS)
Next-generation sequencing changed how we study genes and genomes. It can sequence large stretches of DNA quickly, which makes it useful for broad genetic analysis and research.
NGS gives a deeper view of genetic variation. It can support whole-genome sequencing and help uncover rare mutations. Researchers use it to find disease markers and identify possible therapeutic targets. That flexibility makes it highly valuable in personalized medicine.
Some major benefits of NGS include:
- high-throughput data collection
- detailed genetic insight
- flexible sequencing options
NGS supports precision medicine by helping identify genetic risk and disease-driving mutations. It also supports the development of targeted therapies. As the technology improves, its value in diagnostics and healthcare research continues to grow.

Microarray Analysis
Microarray analysis helps scientists study gene expression on a large scale. It can assess thousands of genes at the same time, which makes it useful for spotting changes in gene activity under different conditions.
Microarrays use small probes fixed to a solid surface. These probes bind to complementary DNA or RNA sequences, which lets researchers measure expression patterns. This technique is used in areas such as cancer research, biomarker discovery, and drug development.
Main features of microarray analysis include:
- assessment of many genes at once
- detection of gene expression changes
- use in biomarker discovery
Microarray technology still plays an important role in genomic research because it can handle large volumes of data efficiently and help explain complex biological systems.
Fluorescence In Situ Hybridization (FISH)
FISH uses fluorescent probes to detect specific DNA sequences on chromosomes. It lets clinicians and researchers see genetic material directly in cells, which makes it useful for diagnosing chromosomal abnormalities and genetic disease.
FISH is highly specific and flexible. It is especially useful for finding structural chromosome changes and identifying defined DNA targets.
Key aspects of FISH include:
- fluorescent probe-based detection
- targeted analysis of genetic material
- use in identifying chromosomal abnormalities
FISH remains a trusted tool in clinical settings because it gives clear, direct results that support diagnosis and treatment planning.

Isothermal Amplification Techniques
Isothermal amplification is an alternative to PCR. Instead of cycling through different temperatures, it amplifies DNA at one constant temperature. That makes it simpler and faster in some settings.
This method is flexible and can be used for single nucleic acids or larger targets. Techniques such as loop-mediated amplification fall into this group. They are often used in pathogen detection and infectious disease testing.
Important features of isothermal amplification include:
- constant-temperature DNA amplification
- fast and simple workflow
- strong use case in infectious disease detection
These techniques are especially useful where full lab infrastructure is not available. Because they are quick and practical, they can support faster clinical decisions and better disease control.
Applications of Molecular Diagnostics
Molecular diagnostics plays a major role in modern healthcare because it helps detect disease early. Early detection can slow or prevent disease progression and gives clinicians more time to choose the right treatment.
In clinical diagnostics, molecular tools help identify infectious pathogens with more precision. Instead of relying on broad assumptions, labs can pinpoint the actual virus or bacterium causing infection. That helps clinicians choose the right therapy.
The field also extends well beyond infectious disease. In oncology, molecular diagnostics helps identify cancer-linked mutations, track treatment response, and detect minimal residual disease. That improves how cancer is managed over time.
Applications of molecular diagnostics include:
- detection of genetic disorders
- disease surveillance and epidemiology
- monitoring of treatment response
These tools also matter in personalized medicine. They help group patients more accurately in clinical trials and support more targeted care across many medical fields.

Role in Precision Medicine and Personalized Healthcare
Molecular diagnostics sits at the center of precision medicine. The goal is to match treatment to the individual patient rather than rely on a one-size-fits-all approach. By looking at a patient’s genetic profile, clinicians can make more informed treatment choices.
Personalized healthcare uses this data to guide therapy selection. It can account for genetic differences that affect how a patient responds to drugs. That helps reduce side effects and improve treatment results.
The benefits include:
- personalized drug selection
- targeted cancer treatment
- risk assessment for inherited disease
This shift has changed healthcare in a meaningful way. Patients can now receive care that better matches their own biology, which improves outcomes.
Biomarker Analysis and Genetic Testing
Biomarker analysis is a key part of disease diagnosis and monitoring. Biomarkers can point to the presence of disease, show whether it is getting worse, or indicate how a patient is responding to treatment. Molecular diagnostics makes it possible to detect these markers with high precision.
Genetic testing looks directly at DNA to identify inherited disorders and disease risk. It can reveal predisposition to certain conditions and support earlier action and better-informed health decisions.
Common uses of biomarker analysis and genetic testing include:
- cancer detection and monitoring
- cardiovascular risk assessment
- prenatal screening
These tools help make healthcare more proactive. When risk or disease is found earlier, intervention can happen sooner.

Advantages and Limitations of Molecular Diagnostic Tools
Molecular diagnostics offers major benefits. It provides fast, precise results and can detect disease at an early stage, which often improves treatment success.
There are still real limits. These tools can be expensive, which affects access. They also require trained staff to run tests and interpret results correctly.
Important considerations include:
- high operating costs
- need for skilled personnel
- risk of false positives in some settings
The challenge is to keep the benefits while reducing these barriers. New advances are pushing the field in that direction, which should make molecular diagnostics more accessible and dependable over time.
Future Trends in Molecular Diagnostics
Molecular diagnostics is still evolving quickly. New tools and methods are making tests faster, cheaper, and more efficient.
Some of the main trends include:
- use of AI and machine learning
- growth of point-of-care testing
- expansion of molecular imaging
Automation and digital health tools are also gaining ground. Together, these changes are reshaping healthcare diagnostics. The direction is clear: faster answers, better precision, and broader access. As these trends continue, molecular diagnostics will take on an even larger role in patient care.

Conclusion
Molecular diagnostic techniques have become a core part of modern medicine. They help clinicians understand disease with more precision and act earlier with better information.
As science and technology keep moving, molecular diagnostics will keep improving too. Its role in clinical care will only grow, especially as treatment becomes more personalized. Better tools should lead to better outcomes, and that makes this field one of the most important parts of modern healthcare.




.webp)
.png)

























.webp)
.webp)