How do molecular diagnostics impact clinical decision-making?
Molecular diagnostics are changing healthcare. They help clinicians diagnose and monitor disease by analyzing biological markers. That makes care more personal, since treatment can be matched to a patient’s genetic profile.
Clinical genomics is one part of this work. It looks at how genetic information affects disease. It can detect mutations that shape treatment decisions, which helps clinicians choose care with more precision.
Biomarker analysis and genetic testing also play a central role. They help show whether a disease is present, how it is progressing, and how it may respond to treatment. That gives clinicians better data and supports more accurate decisions.
This field keeps moving fast. Better tools support earlier detection and, in many cases, better outcomes. As these methods become part of routine care, they are also pushing healthcare toward more preventive and predictive models.

Understanding molecular diagnostics: foundations and technologies
Molecular diagnostics looks at biological markers in the genome and proteome. It helps clinicians understand disease at a molecular level and supports more precise diagnosis and monitoring.
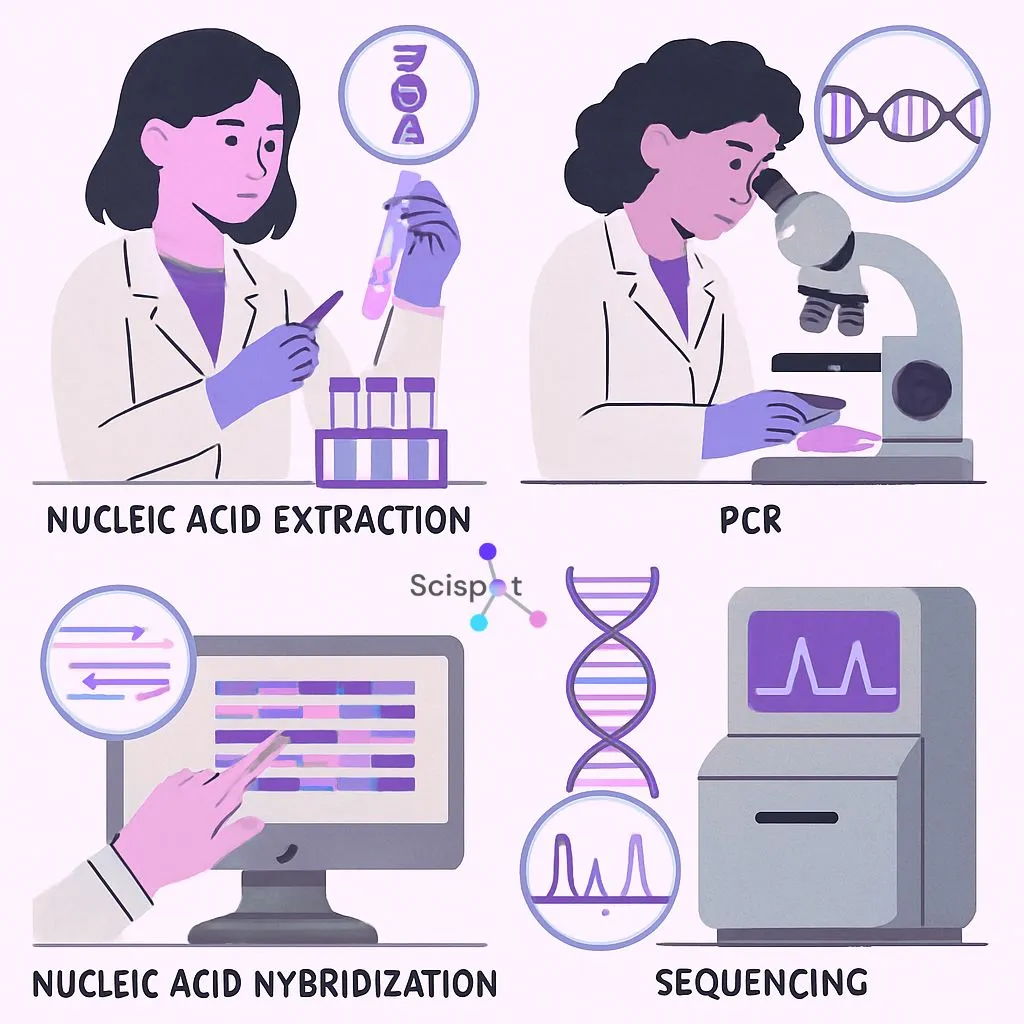
Several technologies sit at the core of this field. These include polymerase chain reaction, next-generation sequencing, and microarrays. Together, they allow detailed analysis of genetic material and help detect mutations and genetic disorders with high efficiency.
A few key techniques include:
- PCR: Amplifies very small DNA samples for closer analysis
- Next-generation sequencing: Supports detailed, high-throughput genetic analysis
- Microarrays: Analyze thousands of genes at the same time
These tools give clinicians information that older methods often miss. They also work well with small sample volumes, which makes them useful in clinical settings. As the technology improves, clinicians get more ways to support targeted treatment.
The role of molecular diagnostics in personalized healthcare
Molecular diagnostics helps move healthcare toward a more personal model. Instead of giving the same treatment to every patient, clinicians can tailor care to a person’s genetic makeup. That can improve treatment response and lower the risk of side effects.
These tools help identify genetic differences that may affect how a disease behaves or how a patient responds to therapy. With that information, clinicians can make better treatment choices, especially in chronic or complex conditions.
Key parts of personalized healthcare include:
- Targeted therapies: Treatments matched to genetic profiles
- Risk assessment: Finding genetic predispositions early
- Treatment planning: Using genetic data to guide care decisions
As molecular diagnostics becomes more common in practice, care shifts away from a broad, one-size-fits-all model. The result is a more individual approach, with better alignment between the patient and the therapy.

Clinical genomics and genetic testing: transforming patient care
Clinical genomics has changed how clinicians understand disease. By studying a person’s genetic information, it can reveal disease risk, likely progression, and possible treatment paths. That makes earlier and more informed intervention possible.
Genetic testing is a major part of this process. It can identify inherited conditions and other health risks, which makes it useful in both diagnosis and family planning. For some patients, it can also explain conditions that had gone undiagnosed for years.
Some of the main benefits include:
- Disease prevention: Finding risk early enough to act
- Tailored treatments: Matching therapies to genetic profiles
- Family planning: Helping families understand inherited risks
As these tools improve, they continue to sharpen patient care. They help clinicians understand complex disease in more detail and make treatment more specific and efficient.

Biomarker analysis and molecular testing in disease management
Biomarker analysis helps clinicians track disease over time. By identifying molecules linked to a condition, it can show how the disease is changing and whether treatment is working.
Molecular testing adds another layer. It detects specific genetic changes that may affect care. That can help clinicians choose targeted therapies and predict treatment response more accurately. Early detection through these methods can also improve outcomes.
Main benefits include:
- Disease monitoring: Tracking disease stage and treatment response
- Treatment selection: Matching therapy to genetic findings
- Improved outcomes: Supporting more precise care decisions
Together, biomarker analysis and molecular testing support more personalized treatment plans. They help clinicians adjust quickly as the disease changes and make care more responsive.
Precision medicine: tailoring treatments with DNA diagnostics
Precision medicine moves away from broad treatment plans and toward care built for the individual. DNA diagnostics make that possible by identifying genetic changes that can guide treatment.
These diagnostics can show which mutations are driving a disease. That helps clinicians choose therapies that target the right issue, rather than relying on a general approach. It can also reduce side effects by avoiding treatments that are less likely to help.
Key parts of precision medicine include:
- Personalized therapies: Treatment based on patient genetics
- Reduced side effects: More selective treatment choices
- Improved drug efficacy: Better targeting of disease-related mutations
This approach has been especially important in areas like oncology, where targeted treatment can make a major difference. As research continues, DNA diagnostics are likely to become a routine part of care across more specialties.
Diagnostic tools and lab diagnostics: from bench to bedside
Molecular diagnostics depends on advanced lab tools that connect research and clinical care. These tools help clinicians detect disease with more precision and make faster, better-informed decisions.
PCR, next-generation sequencing, and microarrays are among the most widely used technologies. Each has a different role, but all help identify mutations and biomarkers that matter in patient care.
Core tools include:
- PCR: Amplifies DNA for close analysis
- Next-generation sequencing: Enables fast, broad genetic testing
- Microarrays: Examines large numbers of genes at once
These tools help move discoveries out of the lab and into clinical use. With better diagnostic data, clinicians can start treatment sooner and with more confidence. As the tools improve, the gap between research and real-world care keeps getting smaller.

Real-world impact: case studies and current molecular diagnostics news today
Molecular diagnostics already has a clear effect on patient care. In oncology, genetic profiling has helped guide targeted therapies, improving survival rates and reducing unnecessary side effects. In infectious disease, rapid molecular testing has helped detect pathogens and mutations early, which is critical during outbreaks.
Other areas are seeing gains too. Rare genetic disorders, for example, are now diagnosed with greater speed and accuracy than before.
Current applications include:
- Oncology: Targeted cancer treatment based on genetic findings
- Infectious disease: Fast identification of pathogens and mutations
- Rare genetic disorders: More accurate and timely diagnosis
As new uses emerge, healthcare teams continue to bring these tools into standard practice. Keeping up with molecular diagnostics news helps clinicians respond faster to new evidence, new tools, and new patient needs.

Challenges, ethical considerations, and the future of molecular diagnostics
Molecular diagnostics brings clear benefits, but it also comes with real challenges. Access is one of the biggest. Many healthcare systems still lack the infrastructure needed to use advanced diagnostic tools at scale.
There are ethical concerns too. Patient privacy, informed consent, and the risk of genetic discrimination all need careful attention. Protecting patient data matters, and so does being clear about how that data is used.
Future progress will likely include:
- AI integration: Faster and more accurate analysis
- Broader access: Wider availability of diagnostic tools
- Stronger data security: Better protection for sensitive information
The future of this field will depend not only on better technology, but also on how well healthcare systems handle access, trust, and ethics.

Conclusion: the evolving landscape of clinical decision-making
Molecular diagnostics is changing how clinicians make decisions. It gives them more precise data, supports earlier detection, and helps match treatment to the patient.
As these tools improve, precision medicine will become a more normal part of care. That can lead to better treatment results, lower costs, and a better experience for patients. Over time, this shift will help make healthcare more predictive, preventive, and personal.




.webp)
.png)

























.webp)
.webp)